TEMPOROMANDIBULAR JOINT (NORMAL ANATOMY AND ITS DISORDERS)PART TWO
TMJ normal anatomy and disorder

Muscles and Movements
TMJ is associated with various muscles which have the purpose of moving and protecting the joint itself.
Masseter, internal, lateral, orexternal pterygoid are the muscles that function to close the jaw.
The muscles which open the jaw are pterygoid medial or internal, geniohyoideus,mylohyoideus , digastric.
There are four muscles which make direct contact with TMJ are masseter, temporal, and two pterygoids.
The muscle masseter with its perimysium has direct contact with the front edge of the articular disc, It originates with several muscular layers from the zygomatic arch and inserts on the branch of the mandible (lateral surface) and coronoid (lateral surface) process, The primary purpose is to raise the jaw.
The temporalis muscle originates from the skull’s temporal fossa and the medial
face of the zygomatic process, it inserts on the mandibular coronoid process, As
with the previous muscle, the temporalis also makes anterior contact with the
articular bone, It elevates the mandible.
The lateral or outer pterygoid muscle is made up of an upper head and a lower ,
The upper bundle originates from the extracranial face of the large sphenoid wing to be inserted in the upper portion of the pterygoid fovea anteromedially to the joint capsule and/or the anteromedial face of the condyle arm ,It touches on the
anteromedial part of the disc, The inferior head originates from the lateral part of the sphenoid pterygoid lamina and is inserted into the pterygoid fovea.
Bilateral activation of the external pterygoid protrudes the mandible which, when activated independently, causes the mandibular bone to deviate contralaterally laterally , In the opening phase of the mouth, the outer pterygoid muscle pushes the condyle forward, in the closing process, it moves the disc anteromedially, The two upper and lower bundles are involved both in the early opening stages and in the early closing stages of the mouth, The internal or medial pterygoid muscle has
its origin in the pterygoid fossa, Through the pyramidal layer of the palatine and
the maxillary tuberosity to the medial angle and mandibular branch, The inner
pterygoid muscle elevates and protrudes the mandible.
TMJ’s complex movements allow for multiple functions
Tweet, Sucking in,Swallow ,Phoning,Expressed facially, Airborne ,Outpouring, retrusion, jaw, lateralization, and Maintain right middle ear pressure(7) .
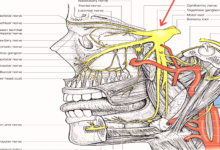
Nerve And Blood Supply
The mandibular nerve (third branch of the trigeminal nerve) provides the TMJ ‘s principal nerve supply.
Additional innervation arises from the deep temporal nerves and the masseteric nerves, The synovial development is induced by parasympathetic otic ganglion fibres, Sympathetic neurons from the upper cervical ganglion reach the joint along the vessels, and play a role in pain reception and blood volume monitoring.
Branches of the external carotid artery, predominantly the superficial temporal
branch, provide its arterial blood supply, Certain branches of the outer carotid
artery, including the deep auricular artery, anterior tympanic artery, ascending pharyngeal artery, and maxillary artery, may also contribute to the joint’s arterial blood supply(8) .
Temporomandibular Disorder (TMD) is a broad term encompassing temporomandibular joint disorders and their associated anatomical structures,
The disorder may be intra-articular due to inflammation, internal structural
changes (internal derangement) or degeneration, or it may be extra-articular due to jaw muscle imbalance or overactivity, Commonly chewing muscles or cervical muscles, There is a strong correlation between cervical column postural dysfunction and TMD , There are numerous other conditions in the TMJ region which may cause pain, To ensure that the right care is provided and potentially significant conditions are not ignored, it is necessary to make an accurate diagnosis.
Anatomy of a TMJ
In an early study on postmortem specimens, it found that the lateral pterygoid muscle was connected to the medial aspect of the joint capsule,
meniscus and the condyle pterygoid fovea in more than half of the specimens, The muscle may have a particular contribution to the TMD, it suggested(9).
Causes of TMD
Intra-Articular Causes
- Inflammatory reactions within the joint
often result from direct trauma, such as a chin blow, indirect trauma, such as
(bruxism), jaw clenching . - Synovitis-It can inflammate the synovium or the capsule, At the end of the spectrum, pain also occurs at rest and reduced spectrum of discomfort.
- Retrodiscitis The retrodisc tissue (a posterior attachment of the articular disk to the mandibular fossa) is highly vascular and inward-looking, and
can cause severe pain if inflamed . - Internal derangement defines situations in which structural changes occur within
the joint, This can be due to direct trauma or indirect trAuma, or prolonged opening of the mouth. - Disc displacement with reduction , The articular disk can be
displaced in any direction, but most commonly moves forward , During opening the disk will be moved forward and bunched up, The disc may reposition or raising itself at a certain point in range creating an audible or noticeable click, The jaw often deviates towards the side that is affected. - Disc displacement without reduction , The disc will not reduce in this more severe version causing pain and a loss of range, This is known as closed door, The jaw often deviates towards the side that is affected, There will be no click but at the time their jaw was locked the patient may report that there was a click there.
- Arthropology- Degenerative Arthritis can be present in the TMJ, It can also be seen as a flattening of the condylar head on plain x-ray or OPG.
- Hyper mobility can lead to excessive anterior jaw and articular disc movement, This will cause the jaw to deviate away from the affected side, The TMJ usually has some clicking sounds, and there may or may not be discomfort.
Extra-Articular Causes
Muscle spasm can cause considerable pain and limited jaw movement.
Cervical postural disorders can bring pain to the jaws, The digastic muscle’s
anterior ventre runs from the chin point to the hyoid bone, This attachment means the digastrics exert a posterior force on the mandible when the head is protracted forward.
Temporary tendonopathy is typically the result of bruxism due to excessivec ontraction of the temporalis muscle.
Mandible fractures often occur at the mandibular symphysis or the neck of the condylar, A fracture of the mandibular symphysis will commonly occur combined with a fracture / dislocation of one or both condyles.
The injury mechanism may be a blow to the jaw, or a fall to the chin (10).
Conclusion
The temporomandibular joint , also known as the mandibular joint, is an ellipsoid variety forming a bicondylar articulation of the right and left synovial joins, The typical characteristics of the synovial joints shown by this joint include a fibrous capsule, a disc, synovial membrane, fluid, and adjacent tough ligaments.
Not only is the mandible a single bone but the cranium is also mechanically a single stable component, hence, the craniomandibular articulation is the appropriate terminology for the joint.
Magnetic resonance imaging has been shown to precisely delineate the
TMJ structures and is the best technique for correlating and comparing TMJ components with autopsy specimens such as bone, disk, fluid, capsule, and ligaments.
Temporomandibular disorders (TMD) are a heterogeneous group of diagnoses that affect the temporomandibular joint (TMJ) and tissues that surround it.
refernces
7-Bravetti P, Membre H, El Haddioui A, Gérard H, Fyad J, Mahler P et al.
Histological study of the human temporo-mandibular joint and its surrounding muscles. Surgical and Radiologic Anatomy. 2004;26(5):371-378.
8-Sessle B, Hu J, Cairns B. Brainstem Mechanisms Underlying
Temporomandibular Joint and Masticatory Muscle Pain. Journal of
Musculoskeletal Pain. 1999;7(1-2):161-169.
9-Peterson L, Naidoo L. Lateral pterygoid muscle and its relationship to the
meniscus of the temporomandibular joint. Oral Surgery, Oral Medicine, Oral
Pathology, Oral Radiology, and Endodontology. 1996;82(1):4-9.
10- Temporomandibular Disorders [Internet]. Physiopedia. 2020 [cited 30 May
2020]. Available from: https://physio-
pedia.com/Temporomandibular_Disorders#cite_note-Balasubramanium-2